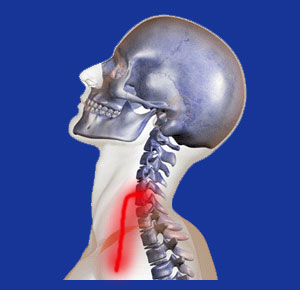
Cervical nerve compression describes a definitive pinched nerve condition that is generating pain and/or other neurological symptoms. Compression is the worst physical condition for a nerve, since it puts the tissue under great duress and prevents proper functionality. Continued compression of any nerve tissue will likely create chronic symptomology, but the symptomatic expressions likely to be produced are quite different than the popular and even basic medical expectations.
Neurological compression is a worse diagnosis than neurological impingement, since it denotes that the tissue is already restricted in its ability to signal, instead of merely being crowded, effaced, displaced and slightly affected by minor mass effect. The proper diagnostic classification is compressive neuropathy and not radiculopathy, since the latter condition can come about from many more possible explanations than just simple structural compression.
This essay seeks to elucidate the diagnosis of a nerve compression and separate this particular wording from other similar, yet slightly different, diagnostic nomenclature.
Cervical Nerve Compression Mechanism
The cervical spinal nerve roots exit from the spinal column at each level of the vertebral column. There are 8 sets of cervical neurological roots, stemming from spinal levels C1 to C7. The final cervical nerve exits at the cervicothoracic juncture between C7 and T1. These nerves begin as part of the spinal cord and separate away from the central cord near the location where they will leave the central nervous system and become the building blocks for the peripheral nervous system outside of the spinal column.
When the nerve roots separate off the spinal cord in the neck, they must travel across the lateral recess to the foraminal canal and out through the neuroforamen, also called the foraminal openings. Once they cross through this space, they have succeeded in their egress from the spine and can now branch off the form the nerve tissues that provide motor, sensory and autonomic messages to the remainder of the body. However, it is possible for the nerves to suffer various impediments to this successful egress from the spine. In fact, it is completely normal and expected that typical spinal aging will make their path narrower and possibly even make it impossible for the nerve to traverse the various locations of the cervical spinal anatomy without suffering some degree of impingement or compression.
Nerve root compression is defined as some tissue exerting force against a nerve in such a manner as to impede it from signally properly or at all. There are many reasons for nerve compression to occur in the neck, including various forms of normal and atypical spinal deterioration, injury to the spinal structures or the effects of spinal operations. Regardless of the cause, once compressed, the nerve signals will not travel correctly or at all, creating dysfunction in the areas of the body that are innervated by the compressed nerve tissue.
Nerve Compression Variations
Besides true compression of a nerve, there are lesser variants of diagnostic impingement terminology used, including nerve crowding, nerve effacement, nerve displacement, nerve impression and mass effect on a nerve. The list above progresses in severity from milder to more significant, with the final 2 terms being virtually synonymous for one another. We have already written a major comparative essay called cervical nerve impingement, for those patients or care providers who want a more thorough comparison of each of these forms of diagnostic nomenclature.
Actual and verified nerve compression will produce some form of symptomology, while the above alternate diagnoses will not necessarily produce any expression. However, since the list above progresses in clinical significance, the chances of the patient suffering symptoms from each also increases as one moves forward in the list.
It should be noted that although “pinched nerve” might be the common layman’s term for a cervical nerve compression scenario, the proper medical diagnostic term is compressive neuropathy.
Cervical Nerve Compression Evaluation
In order to separate nerve compression from other forms of nerve impingement that most likely do not produce symptoms, the following guidance should be observed by diagnosticians:
Since nerves usually can not be imaged, it might be impossible to determine if the nerve is actually compressed or not. Doctors must remember that nerves are very small and the degree of foraminal stenosis would have to virtually close-off anatomical openings or passageways in order to definitely compress nerve tissue in most cases.
Clinical symptomatic correlation is a very important step in suspected nerve compression evaluation. Most patients are misdiagnosed because symptomatic correlation is neglected or only partially performed. In most of these patients, there are blatantly obvious discrepancies between the expected symptomology (expression or location) and the actual expressed symptom set. This evidence is either not collected or is arbitrarily ignored, leading to iatrogenic error and abysmal treatment results.
Doctors must always remember the virtually universal nature of most spinal degenerative evidence and the fact that the vast majority of spinal aging does not produce symptoms, even when stenosis reaches levels that require regular monitoring. In essence, just because stenosis exists does not mean it is compressing any nerve tissue.
Finally, and most importantly, the type of symptoms expressed in true compressive neuropathy scenarios usually follow a simple progression beginning with tingling and pain (locally and possibly in innervated location), evolving towards subjective, then objective numbness, followed by weakness in the innervated area and finally, utter dysfunction. If chronic pain endures for an extended timeframe and the symptomology does not progress, it is highly unlikely that the nerve is compressed, even if all other diagnostic parameters check out. This is the single greatest compressive neuropathy-related diagnostic mistake we witness regularly in the back and neck pain treatment arena.
Neck Pain > Pinched Nerve Neck Pain > Cervical Nerve Compression





